With a lot of research investigating the role that sugar reduction, blood sugar management, the microbiota and prebiotics have to play, understanding how they can be used as tools in the fight against obesity is steadily increasing.
There is broad scientific consensus that carbohydrate-based foods with low or reduced glycaemic properties should be the preferred food choice for long-term health. This is supported by approved EU health claims regarding their reduced glycaemic response and by the body of research being reviewed and promoted by the International Carbohydrate Quality Consortium.
The latter group of scientists who work in the area of blood sugar management has concluded that reducing the blood sugar response after intake is a beneficial physiological effect.
Convincing evidence exists that diets that are low in glycaemic index and glycaemic load have health benefits — not only in the management and prevention of diabetes mellitus (improving insulin sensitivity and beta-cell function) and the prevention of coronary heart disease (improving blood lipids and inflammatory markers), but also in terms of weight management (reducing body fat mass).1
Encouraging the reduction of blood sugar levels as a means of supporting weight management makes sense, especially when the role of insulin as a storage hormone and a major driver of post-consumption metabolism is considered.
However, to reduce the glycaemic effect of a food to lower blood sugar levels, a modification or reduction in the glucose supply is required. Modification can be achieved with low glycaemic yet fully available carbohydrates and reduction by using partially or non-available carbohydrates.
Research into the different approaches to lowering blood sugar levels continues to progress. One study by Professor Christiani Jeyakumar Henry et al. looked at lowering blood sugar levels with a slowly released, low glycaemic yet fully available carbohydrate.2
The results demonstrated that participants who followed a low glycaemic diet using a slow release sugar (BENEO’s functional carbohydrate Palatinose), instead of a high glycaemic diet with quickly available sugar, experienced three main improvements: a lower glycaemic profile, reduced variability in blood sugar levels and improved fat burning. These improvements are all aspects of an improved metabolic profile that, with time, can support weight management.
Other research addressed the effects of sugar replacement with prebiotic, soluble dietary fibre. Lightowler et al. showed that blood sugar levels and insulin levels could be markedly reduced with the replacement of sugars with chicory root fibre (Figure 1).3
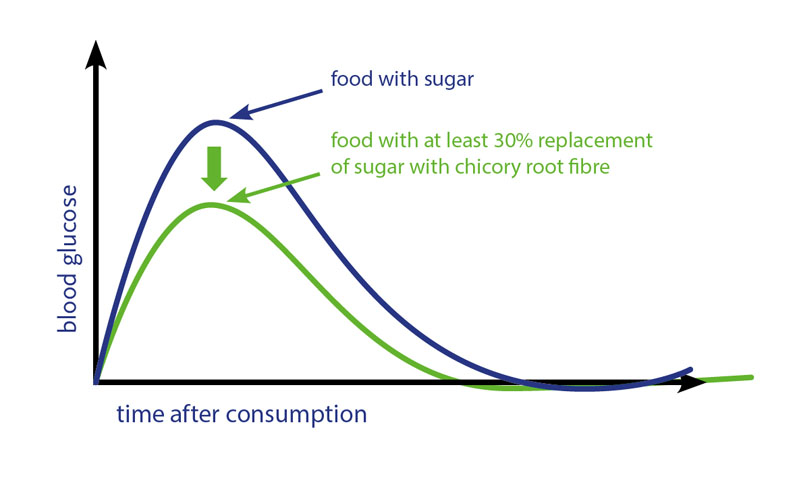
Figure 1: Replacing glycaemic carbohydrates with inulin-type fructans from chicory reduces the postprandial blood glucose and insulin response to foods
The more sugar was replaced with chicory root fibre, the lower the blood glucose response. In addition, for both approaches — sugar replacement with a slow release sugar or with chicory root fibres — corresponding blood sugar-related EU health claims are available.
As well as supporting weight management via lower blood sugar levels, chicory root fibre also has a more direct link to weight management. This is because chicory root fibre inulin and oligofructose are the only plant-based prebiotics available on the market and make up two out of only three existing scientifically proven prebiotics.
Being prebiotic, they create a better-balanced microbiota that, in turn, can influence satiety via the gut-brain axis. Research results by Professor Raylene Reimer et al. showed that oligofructose-enriched inulin (BENEO’s prebiotic chicory fibre, Orafti Synergy1), improves appetite regulation, decreases food intake in overweight and obese children and improves systemic inflammation, helping children to eat less and improve their health, naturally.4
Even in 2014, consumers were already making the link between blood sugar management and health benefits. In a consumer survey by the market research company Insites, consumers cited benefits such as
- feeling nourished and satisfied for longer
- being good for weight management
- helping disease prevention
- offering fewer cravings.5
So, five years on, as waistlines continue to grow across the globe, there is even greater pressure on governments and, in turn, food and drink producers to offer products to consumers that promote long-term health.
With a growing body of research pointing towards blood sugar management as a powerful tool in the war against obesity, and more consumers now realising its potential, the food and drink industry has an opportunity to embrace a wider range of products that promote, rather than hinder, health.
As Simon Capewell, a professor in public health and policy at Liverpool University has said about the obesity epidemic: “This is a preventable catastrophe,” so let’s be part of the solution, not part of the problem.6
References
- L.S. Augustin, et al., “Glycemic Index, Glycemic Load and Glycemic Response: An International Scientific Consensus Summit from the International Carbohydrate Quality Consortium (ICQC),” Nutr. Metab. Cardiovasc. Dis. 25(9), 795–815 (2015).
- C.J. Henry, et al., “A Low Glycaemic Index Diet Incorporating Isomaltulose is Associated with Lower Glycaemic Response and Variability, and Promotes Fat Oxidation in Asians,” Nutrients 9, E473: doi: 10.3390/nu9050473 (2017).
- H. Lightowler, et al., “Replacement of Glycaemic Carbohydrates by Inulin-Type Fructans from Chicory (Oligofructose, Inulin) Reduces the Postprandial Blood Glucose and Insulin Response to Foods: Report of Two Double-Blind, Randomized, Controlled Trials,” Eur. J. Nutr. 57(3), 1259–1268 (2018).
- A. Nicolucci, M. Hume and R. Reimer, “Effect of Prebiotic Fiber-Induced Changes in Gut Microbiota on Adiposity in Obese and Overweight Children,” The FASEB Journal 29(1), Abstract 276.6 (2015): www.fasebj.org/doi/abs/10.1096/fasebj.29.1_supplement.276.6.
- BENEO Blood Glucose Consumer Research: A qualitative survey conducted online with at least 30 participants per country during a 2.5-week period (September–November 2014).
- www.thetimes.co.uk/article/obesity-rate-in-uk-children-doubles-during-primary-school-years-to-top-us-figure-jz0d9txvs.





